
Balancing the Collaboration Equation
Jon Cohen*
Photos by Malcolm Linton
An inside look at three veteran marriages between African AIDS researchers and foreign colleagues illustrates the benefits--and stresses--of partnership
When researchers from the University of Manitoba in Winnipeg, Canada, began seeing an unusual number of cases of genital ulcers in the late 1970s, they turned to colleagues at the University of Nairobi for help. Friendships grew, and in 1980, the Canadians sent a senior infectious disease fellow to Nairobi for a year to study genital ulcer disease, which is relatively common in Kenya. That visit sowed the seeds for the longest running and one of the most productive AIDS research collaborations in Africa.
The project quickly expanded to include a study of sexually transmitted diseases (STDs) among prostitutes in a teeming Nairobi slum called Pumwani. When STD guru King Holmes of the University of Washington, Seattle, joined the project in 1984, a junior fellow working with him, Joan Kreiss, suggested they look into the prevalence of HIV among the prostitutes. Holmes and Manitoba's Frank Plummer, who now presides informally over the collaboration, tried to talk Kreiss out of the idea. They had seen no AIDS cases in Nairobi and thought the work would lead nowhere. Fortunately, Kreiss persisted. "We found that two-thirds of the women in Pumwani were infected with HIV, which was a complete shock to everyone," recalls Plummer. "That turned things around completely."
High-profile AIDS papers began to pour out of the collaboration. They described the extent of the epidemic in Kenya and linked high risk of HIV transmission to genital ulcer disease, contact with prostitutes, and lack of male circumcision. The collaborators discovered--much to the amazement of AIDS researchers around the world--that about 5% of the prostitutes did not become infected with HIV despite repeated exposure, suggesting that their immune systems might hold important clues for AIDS vaccine developers. "Our collaborations have really yielded results that have benefited the world at large," says the University of Nairobi's Elizabeth Ngugi, who started the outreach work with the Pumwani prostitutes.
Given that string of achievements, you might think the Kenya project is a smooth-functioning model of cooperation. But everybody involved will tell you that it has not been easy. Kenyan researchers constantly find themselves balancing their expectations and needs with those of their collaborators, who not only provide the bulk of the funding but also have better access to organizers of conferences, editors at journals, and the international media. "There are equity issues that make it difficult, and it's a constant tension," says Plummer. "The collaboration is like a marriage," adds Job Bwayo, chair of the University of Nairobi's medical microbiology department and head of the AIDS research effort. "You have to give and take."
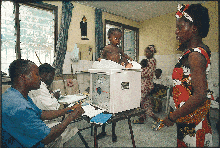
Together we stand. Abidjan's Projet RETRO-CI collaboration, funded by the U.S. CDC, pooled data from studies at this prenatal clinic with those from another similar clinic run by French researchers across town.
Stresses and strains are not unique to the Nairobi partnership. In a dozen projects Science visited across sub-Saharan Africa, tensions are part and parcel of collaborative efforts. Most revolve around equity: access to financial resources and facilities, participation, transfer of technology, self-reliance, training opportunities, and credit. Foreign scientists also on occasion have had to confront their African colleagues about using lab resources to conduct personal business.
Yet, in spite of the difficulties, international collaborations are essential for conducting research in sub-Saharan Africa, where few countries can afford scientific research on AIDS--or anything else, for that matter. Indeed, they account for most of the research on the continent (see p. 2156). Three of the longest running projects--the Nairobi collaboration, a Swedish-Tanzanian project, and a collaboration in Côte d'Ivoire funded by the U.S. Centers for Disease Control and Prevention (CDC)--provide different models of how contrasting research worlds can work productively together.
Staying power
The fact that the Kenya collaboration continues to flourish and produce groundbreaking results after 2 decades suggests that the partners in this marriage are doing something right. Chemistry is an important factor--as it is in most partnerships--and many of the participants credit Plummer with creating the right ambiance. "Frank is a quiet person who doesn't care about quarreling," says Bwayo. "He's been central to this working."
Plummer, a gentle but determined bear of a man with a salt-and-pepper beard, first came to Kenya in 1981 as the second fellow sent out from Manitoba. His 11-month stay led to a dozen papers co-authored with Kenyans, Canadians, and a young Belgian: Peter Piot, who now heads UNAIDS, the Joint United Nations Programme on HIV/AIDS. "I loved the place," says Plummer. "I couldn't wait to get back." He returned in 1984 and has made it home ever since.
The partnership continued to expand, bringing in universities from Seattle, Ghent, Toronto, Oxford, and Rotterdam. One key to its success is that the international partners--who together spend $3.6 million a year on research and another $1.2 million on intervention and training programs--have brought critical resources to the effort. A clinic to this day provides free care and treatment to Pumwani prostitutes. The University of Washington, with funding from the National Institutes of Health's Fogarty International Center, has paid for 48 Kenyans to come to Seattle for advanced training, and a few more have studied at Oxford, Winnipeg, and Antwerp. Kreiss started new studies across the country in Mombasa. The collaboration also built and equipped a lab on the Nairobi campus that has state-of-the-art machinery for doing HIV virology and immunology. "We wouldn't be doing any research without our collaboration," says Bwayo.
The outside collaborators' willingness to listen to the complaints and concerns of their Kenyan partners helps explain the collaboration's survival, too. On 31 January 1998, they got an earful. On that Saturday, 22 researchers from Kenya, the United States, Canada, Belgium, and the Netherlands held a retreat to discuss the collaboration's strengths and weaknesses. A report of that meeting offers a rare peek into the frustrations faced by African scientists--and their wealthier collaborators--all over the continent.
Collaborators, the Kenyans said, should try harder to incorporate Kenyans when they draft research proposals, manuscripts, and conference presentations. University of Nairobi staff who currently do not work with the project should have more opportunities to participate. Collaborators should more freely share their late-model vehicles and computers. Rather than shipping samples out of the country because of a lack of equipment, more technology transfer should occur. The Kenyans also asked their collaborators to share information more freely about their budgets and encourage, rather than criticize, use of the lab for university and even private business.
This soul-searching led to a revised "Statement of Principles" and a list of "expected benefits and mutual obligations." It didn't resolve all the problems, and collaborators challenged many of the criticisms, emphasizing that they had their own frustrations. Yet the collaboration, which has published nearly 300 papers, continues to expand. Recently, the group has started research projects in new communities, launched a project to develop Kenya's first AIDS vaccine, and drawn up plans to construct a new wing at the university.
Long-term survivors
In neighboring Tanzania, a different kind of collaboration between Swedish and Tanzanian researchers, the TANSWED HIV Program, has been flourishing for 14 years. It has resulted in nearly 250 published papers and abstracts. Like most long-standing African AIDS research projects, this one has moved from describing the epidemic to testing interventions to slow HIV's spread, including preparing cohorts for vaccine studies.
"It's a true partnership," says Fred Mhalu, an infectious-disease specialist at Muhimbili University in Dar Es Salaam. "Both sides are benefiting." Gunnel Biberfeld of the Swedish Institute for Infectious Disease Control, who is well known for her AIDS vaccine studies in monkeys, agrees. "It's not one-way," Biberfeld says. "We learn a lot."
In contrast to the relatively freewheeling Nairobi collaboration, TANSWED is tightly structured. The Swedish International Development Cooperation Agency provides most of the funding--$8 million since 1986. It has strict rules designed to encourage technology transfer and discourage empire-building. It prohibits either side from hiring full-time investigators, for example, and doesn't fund new labs for the project. "We don't believe in establishing things separately, but to reinforce what's there," says Biberfeld. "Then it becomes permanent." The project has also provided support for many young Tanzanian researchers to participate in a "sandwich" program that combines brief training in Sweden with studies in Tanzania--a model that aims to reduce the risk of students staying abroad.
These policies draw mixed reviews from the participants. Biberfeld says the prohibition on Swedish researchers working full-time in Tanzania slows down research and discourages Swedish investigators from participating. But Mhalu likes the policy. It encourages more Tanzanians to do the fieldwork, he says, and it helps eke out scarce resources. Full-time Swedish investigators, he notes, would eat up a big chunk of the budget. "I've seen several other projects that had to shut down because of how much they spend on [foreign scientists]," says Mhalu.
On the other hand, neither side likes the ban on hiring full-time Tanzanians. "Our project has 30 scientists who have to teach, do clerical work, and don't have full-time research assistants," says Mhalu, whose salary and lab space is paid for by the Tanzanian government.
Biberfeld stresses that, at the end of the day, "this is a Tanzanian project." Not only do the Tanzanians have nearly twice as many principal investigators as the Swedes, Tanzanians routinely present the data at international conferences and receive top billing in publications.
A tale of one city
Across the continent in Côte d'Ivoire, a French-speaking country on Africa's west coast, two large, often overlapping AIDS research projects coexist in the bustling city of Abidjan. The U.S. CDC funds the larger one, Projet RETRO-CI, while France's National Agency for Research on AIDS supports the other.
Projet RETRO-CI, in collaboration with the Ivoirian Ministry of Health, set up shop in 1988, studying basic epidemiology of both HIV-1 and the less understood HIV-2, which is largely confined to western Africa. The CDC researchers and their Ivoirian collaborators were soon publishing their findings in high-profile journals, including Science. "It was lucky initially that we asked simple questions," says CDC's Kevin DeCock, Projet RETRO-CI's first director.
Like the Nairobi collaboration, RETRO-CI has brought critical resources to the project, including establishing a topflight lab (see profile on p. 2157), a clinic that provides free health care to sex workers, and a training program for African researchers. RETRO-CI, unlike TANSWED, has 135 full-time staff, but CDC limits the number of U.S. scientists (there are now only two), and African scientists are encouraged to publish papers and present at meetings. Yet the initial reception in Côte d'Ivoire was mixed. "When we started, people said, 'What are you doing, research is not very important,' " recalls Ehounou Ekpini, the project's deputy director.
Project RETRO-CI staff had a mixed reaction themselves in 1994 when French AIDS researchers, fleeing the Rwandan genocide, established another program in Abidjan. But after some initial wariness, the two groups began working together. In 1998, they pooled data on mother-to-child transmission of HIV during the postnatal period, and last year, they published back-to-back complementary papers in The Lancet demonstrating that cotrimoxazole, a relatively cheap sulfa drug, can decrease disease and prolong the lives of HIV-infected people. CDC's Stefan Wiktor, who stepped down as Projet RETRO-CI's director in August, has come to see the relationship as mutually beneficial. "It looks funny for people to do similar studies in the same city, but it's worked out well," Wiktor says. "And among Ivoirians, they don't view it as a problem."
Issa Malick Coulibaly, who until last year headed the country's National AIDS/STD/TB program, says the intense research interest in Côte d'Ivoire has transferred much technology to his country. "We need to have a good capacity for research," says Coulibaly. "We don't need to take blood of people living here and send it to France and the CDC."
As much as African countries want to build their research infrastructures, ultimately, the collaborations in Kenya, Tanzania, Côte d'Ivoire, and elsewhere won't be judged by how much they strengthen research, but by how much the research findings help prevent HIV and AIDS in these countries. And on that score, everyone is still struggling. "One of the frustrations I felt at the end of my stay here was lack of translation of research findings to public health programs," says Wiktor. "Research isn't enough."
* Jon Cohen was accompanied by photographer Malcolm Linton. For a gallery of additional photos and the stories behind them, see
www.sciencemag.org/feature/data/aids_africa/gallery.shl.
Volume 288,
Number 5474,
Issue of 23 Jun 2000,
pp. 2155-2159.
Copyright © 2000 by The American Association for the Advancement of Science.
|